What’s in a Lens?


July 24, 2023
What’s in a Lens? Comparing the Human Crystalline Lens, Implantable Collamer Lenses (ICLs), and Intraocular Lenses (IOLs)
The field of ophthalmology has witnessed remarkable advancements in lens technology over the years, revolutionizing the way we address vision impairments. Modern implantable options such as implantable collamer lenses and intraocular lens implants are made of unique materials that bring exceptional benefits to patients seeking improved vision. In this blog post, we’ll explore the differences in composition and characteristics of lenses, including the lens we’re born with- the human crystalline lens.
Human Crystalline Lens
The human eye houses a biconvex crystalline lens that’s located behind the iris and in front of the vitreous humor. The lens, along with the cornea, is responsible for focusing incident light rays. Composed primarily of transparent proteins called crystallins, the lens allows for precise accommodation and adjustment of focal length, enabling clear vision at various distances. It is unique in that its protein content – nearly 60%- is higher than almost any other tissue in the body! The lens also gets heavier over time: weighing in at 65 mg at birth and increasing in weight to 160 mg by the age of 10, and 250 mg by the age of 90.
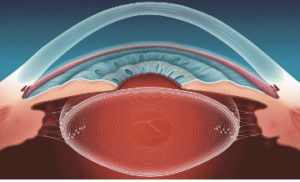
The body of the lens is surrounded by a capsule, which acts as a barrier and contributes to shaping the lens during accommodation (focusing on near objects). The capsule is made up of type IV and type XVIII collagen and a precise array of compounds including laminin, entactin, perlecan, heparin sulfate proteoglycan, and fibronectin.
As we age, the crystalline lens gradually loses its flexibility and transparency, and there is a gradual increase in yellowish pigmentation. It’s hypothesized that the yellowing of the lens is due to the production of 3-hydroxykynurenine and other metabolites of tryptophan that filter UV light.
Implantable Collamer Lenses (ICLs)
Implantable Collamer Lenses, also known as “phakic intraocular lenses”, are advanced lens implants designed to correct vision in individuals with refractive errors such as myopia and astigmatism. Unlike intraocular lenses, ICLs are implanted in front of the eye’s natural lens, preserving its accommodative ability. Composed of a collagen copolymer material known as collamer, these lenses offer exceptional optical clarity, UV protection, and excellent biocompatibility.
What exactly is “collamer”? Collamer is a blend of polymer and collagen made of 60% poly- hydroxyethyl methacrylate (HEMA), water (36%), and benzophenone (3.8%) and 0.2% porcine collagen. This combination of materials makes the lens light and hydrophilic and allows for exchange of gas and nutrients throughout the anterior chamber of the eye. The lens also has an ultraviolet absorbing chromophore.

At SharpeVision, we exclusively use the EVO ICL, which is a rectangular one-piece plate-haptic design plano-concave ICL with a central port. The lens is available in four lengths (12.1, 12.6, 13.2, and 13.7 mm). The most notable feature of the EVO is its central port (hole) of 0.36 mm (KS-Aquaport) which eliminates the need for a Nd:YAG iridotomy laser procedure that was previously required in patients who had the older model Visian ICLs implanted. The port supports swift circulation of the aqueous humor.
Thanks to their flexible design, ICLs can be implanted (and explanted) through a small corneal incision, making them a reversible and customizable option for individuals seeking vision correction.
Intraocular Lens (IOL) Implants
Intraocular lens implants have become the standard of care for patients seeking elective vision correction over age 50 and those undergoing cataract surgery. These artificial lenses replace the clouded or dysfunctional natural lens, restoring visual clarity at one or more focal points.
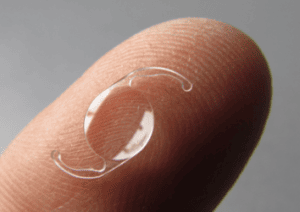
The first intraocular lenses (IOLs) were manufactured in 1949 and made of rigid plastic—namely, polymethyl methacrylate (PMMA)— this biomaterial was the only one available for IOL implantation for over 30 years. Like in many industries, research and development of new materials has transformed the field of surgical ophthalmology. Modern IOLs are typically made of newer, safer and more durable biocompatible materials like hydrogel, silicone, acrylic and acrylate.
IOLs come in various designs, including monofocal lenses that provide clear vision at a fixed distance, toric lenses that correct astigmatism, and multifocal lenses that enable vision at a range of different distances. Like ICLs, some advanced IOLs even incorporate technology to filter out harmful blue light and provide enhanced visual outcomes. With advancements in surgical techniques, these lenses can be implanted through laser assisted micro-incisions, promoting faster recovery and improved postoperative outcomes.
Is it possible for my eye to reject the lens? Will the lens last forever?
Intraocular lenses (IOL’s) are made to be biocompatible and designed to last a lifetime, so the body will not reject them, and they can safely stay in the eyes for the duration of one’s life.
Can the lens move once it is implanted?
It is possible for the lens to dislocate. This may occur as a result of trauma, infection, inflammation or other conditions which weaken the connections (zonules) that hold the lens in place. Be sure to see your doctor if you experience any changes in vision following cataract surgery.
How do I choose the right lens for me?
The choice of lens depends on the specific needs of the patient and requires careful consideration with respect to desired outcome. With ongoing advancements in lens technology, the future holds exciting prospects for even more innovative solutions, enhancing the lives of individuals seeking improved visual acuity.
References
- Alfonso JF, Fernández-Vega-Cueto L, Alfonso-Bartolozzi B, Montés-Micó R, Fernández-Vega L. Five-year follow-up of correction of myopia: Posterior chamber phakic intraocular lens with a central port design. J Refract Surg. 2019;35(3):169-176. doi:10.3928/1081597X-20190118-01.
- Hejtmancik JF, Shiels A. Overview of the Lens. Prog Mol Biol Transl Sci. 2015;134:119-127. doi:10.1016/bs.pmbts.2015.04.006
- Lovisolo CF, Reinstein DZ. Phakic intraocular lenses. Surv Ophthalmol. 2005;50(6):549-587. doi:10.1016/j.survophthal.2005.08.011
- Salmon, J. F., & Kanski, J. J. (2020). Kanski’s Clinical ophthalmology: A systematic approach (9th ed.). Edinburgh: Elsevier Limited.
- Zhong, X., Long, E., Chen, W. et al. Comparisons of the in-the-bag stabilities of single-piece and three-piece intraocular lenses for age-related cataract patients: a randomized controlled trial. BMC Ophthalmol 16, 100

Dr. Matthew R. Sharpe