Understanding Corneal Cross-Linking
A Potentially Life-Changing Treatment for Keratoconus or other types of Corneal Ectasia (Weakening)

May 8, 2024
Corneal cross-linking is a relatively new, minimally invasive procedure used to treat progressive keratoconus and other conditions that weaken the cornea. The goal of the treatment is to strengthen the corneal structure, thereby stabilizing its shape and preventing further deterioration. In this blog post, we will explore what corneal cross-linking is, how it works, its benefits, and what to expect during and after the procedure.
What is Keratoconus?
Keratoconus (KCN) is a condition where the cornea, the clear front part of the eye, becomes thin and bulges outward in a cone-like shape. It can be compared to a bulge in a tire or a balloon. The pressure in the eye causes the cornea to stretch, or thin out. This abnormal curvature can cause distorted vision, nearsightedness, irregular astigmatism that can’t be corrected with glasses. The exact cause of keratoconus is not well understood, but genetic and environmental factors are believed to play a role. More recent theory is that chronic eye rubbing may play a part in the tissue stretching and thinning. People who have eye allergies, people with Down Syndrome who rub their eyes habitually are also at risk. Those with sleep apnea who may sleep with their fists or forearms pressing into their eye socket may also cause this stretching. Historically, treatment has been scleral contact lenses, which are large, rigid, uncomfortable contact lenses that act like a brace to hold the cornea where it is, as well as provide a regular front curvature of the eye to improve vision. End-stage KCN can cause stretching to the point of needing a corneal transplant.
Forme Fruste KCN
Forme Fruste KCN is the term for patients whose corneas have some of the signs of KCN, but in a milder form. To determine if a patient has this condition we look at numerous factors: the patient age, the corneal asymmetry in curvature from top to bottom, the posterior surface of the cornea and how much bulging it has, the corneal thickness, the direction of the astigmatism, the refractive error (also called the prescription or degree of nearsightedness). At SHARPEVISION, we screen every patient who comes seeking vision correction surgery for KCN and its milder forms. We see milder forms of corneal irregularity that are on a spectrum of severity. I estimate that it’s about 1% of all the patients that we screen that are not candidates for corneal refractive surgery such as LASIK or PRK. For those patients we can potentially perform EVO implantable contact lenses (ICL) which do not alter the cornea. If needed, we can perform CXL prior to EVO ICL. See our blogpost on EVO: https://sharpe-vision.
What is Corneal Cross-Linking?
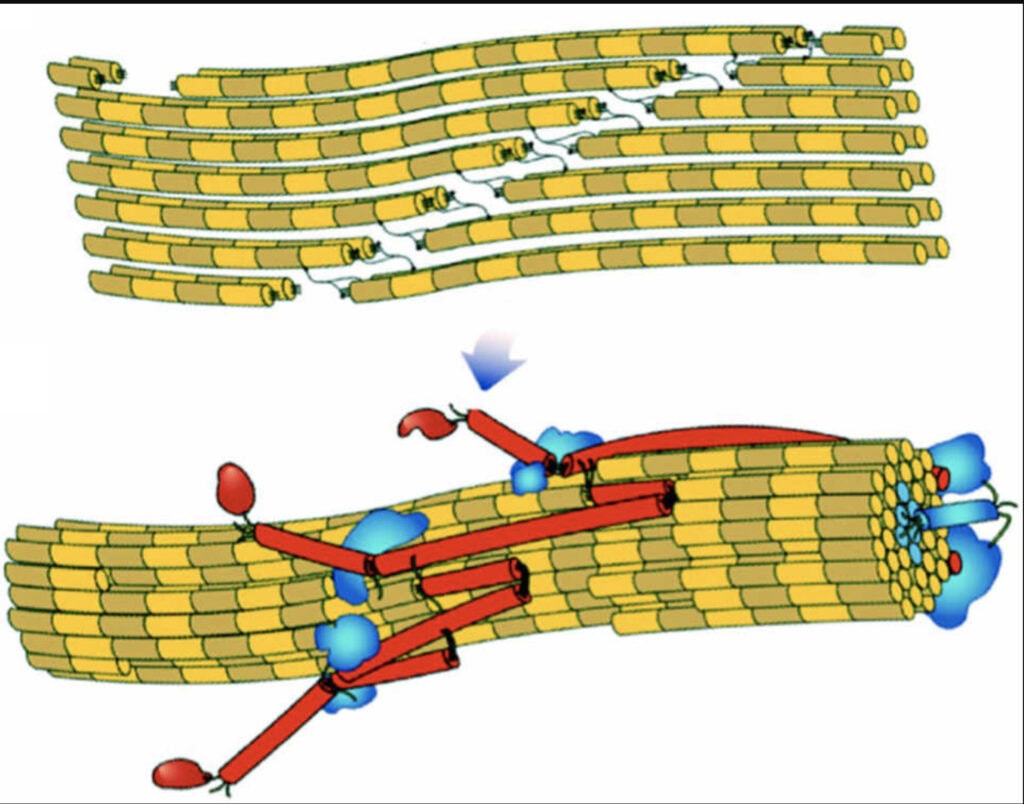
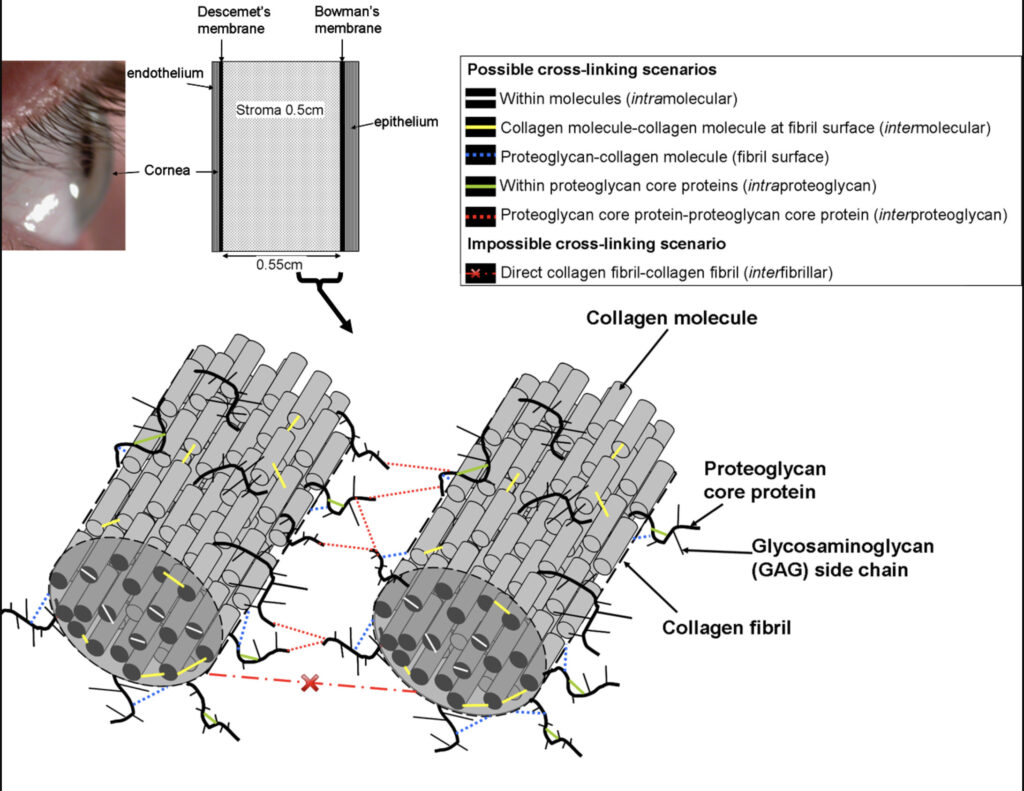
Corneal cross-linking (CXL) is a treatment designed to strengthen the cornea and prevent further deterioration in conditions like keratoconus. The term “cross-linking” refers to the creation of chemical bonds between collagen fibers within the different bands, or layers of the cornea. By increasing the cross-linking of these fibers, the cornea becomes stronger, and less likely to change shape. Think of the cornea like a sheet of plywood. There are many layers of collagen that are “glued” together in the cornea. Corneal cross linking increases the “glue” between layers, thereby strengthening the cornea. The cornea becomes more rigid, stronger, and less likely to have the layers slide and stretch.
There are two primary types of corneal cross-linking:
1. Epithelium-On (Transepithelial) CXL: In this method, the epithelium, the surface skin layer of the cornea, is left intact. This approach has a quicker recovery time, and is less uncomfortable. By leaving the epithelium on, the recovery is easier, but questions remain as to whether it can be equally as effective as the technique of removing the epithelium. The penetration of the riboflavin solution into the collagen layers below the epithelium may be restricted.
2. Epithelium-Off (Standard) CXL: In this method, the epithelium is removed to allow better penetration of riboflavin into the cornea. This method is more common and generally considered more effective for treating keratoconus. This was the original method, and what is currently FDA approved. The recovery is similar to PRK surgery where the corneal epithelium, or “skin” layer has to grow back over the 8mm circle of tissue that is removed. There is discomfort (few patients say “pain”) for about 48-72 hours, vision recovers slowly over 6-8 weeks. Corneal topography (measurements of the corneal shape, thickness, symmetry) are performed serially to ensure stability.
How Does Corneal Cross-Linking Work?
The process begins with numbing your eyes with eye drops. The corneal epithelium is then removed, and specially formulated riboflavin (vitamin B2) eye drops are applied to the cornea. Riboflavin is a photosensitizer, which means it reacts to light in a way that facilitates cross-linking. After the riboflavin has sufficiently penetrated the cornea, a controlled dose of ultraviolet (UV) light is used to activate the riboflavin, creating new cross-links within the collagen fibers. This process takes about 90 minutes. A contact lens is placed on the surface of your eyes, and antibiotic/steroid combination drops are applied. Pain medicine is dispensed to cover you for post-operative pain that typically lasts 48-72 hours. The contact lens is removed at 5 days postoperatively. Eye drops are continued for 1-4 weeks, and follow ups are scheduled over the first year or more to ensure stability and good healing.
Benefits of Corneal Cross-Linking
The primary benefit of corneal cross-linking is its ability to halt or slow the progression of keratoconus, reducing the need for corneal transplants and other more invasive procedures. Additional benefits include:
Improved Corneal Stability: Cross-linking and strengthens the cornea, making it less prone to further bulging.
Reduced Need for Corrective Lenses: By stabilizing the cornea, cross-linking can lead to improvements in vision, reducing dependence on glasses or contact lenses. After stabilizing the cornea, one may potentially be considered for vision correction surgery.
Minimally Invasive: CXL is an outpatient procedure, usually taking about 60 to 90 minutes, with minimal risk of complications.
What to Expect During & After the Procedure
Corneal cross-linking is typically performed in a clinic or hospital setting. Before the procedure, patients will receive numbing drops to numb the eye. During the treatment, patients will lie back, and the riboflavin drops will be applied to the eye. The UV light is then used for about 30 minutes to activate the riboflavin.
After the procedure, patients might experience some discomfort, light sensitivity, and a sensation of having something in the eye. These symptoms are generally mild and resolve within a few days. Patients may be prescribed antibiotic and anti-inflammatory eye drops to aid healing and prevent infection.
In terms of recovery, most patients can return to their regular activities within a week, but full visual stabilization may take a few weeks to months. During this period, it’s important to follow the post-procedure instructions provided by the eye care professional to ensure proper healing.
Who is a Candidate for Corneal Cross-Linking?
Corneal cross-linking is primarily used to treat keratoconus, but it may also be suitable for other conditions that weaken the cornea, such as pellucid marginal degeneration or post-LASIK ectasia. Ideal candidates are those who have a progressive condition and are experiencing changes in vision due to corneal distortion.
Risks of CXL
The corneal cross linking procedure does have a few rare complications, or risks. Perhaps the biggest one is corneal infection which could lead to scarring or loss of best corrected vision and even corneal transplant. This is extremely rare with laser vision correction, perhaps one in 10,000. The numbers of patients receiving corneal cross-linking are too small so far to get any large numbers to determine risk of infection, but it might be expected to be comparable to vision correction surgery. Another risk is corneal haze or scarring which is also extremely unlikely, but could adversely affect you visual acuity and cause glare, haloes, starbursts, or other decreases to your vision. Another risk is that CXL might be that it is ineffective and that your corneal weakening and stretching progress. These numbers are all anecdotal at this point, although the numbers of people receiving this new procedure are growing, and the potential alternatives (corneal transplant) make CXL well worth the small risks.
Conclusion
Corneal cross-linking has revolutionized the treatment of keratoconus and similar conditions, offering a minimally invasive option that can stabilize the cornea and improve visual outcomes. If you suspect you have keratoconus or have been diagnosed with it, discuss with your eye care professional whether corneal cross-linking could be a suitable treatment option for you. It should be done without delay, because KCN and other corneal ectasias are progressive. CXL is meant to stabilize, not reverse the condition, although sometimes improvement does occur. The procedure’s potential to stabilize and even improve vision makes it a valuable tool in the fight against corneal disorders.
Treatment of Progressive Keratoconus
Treatment of Corneal Ectasia Following Refractive Surgery

Dr. Matthew R. Sharpe